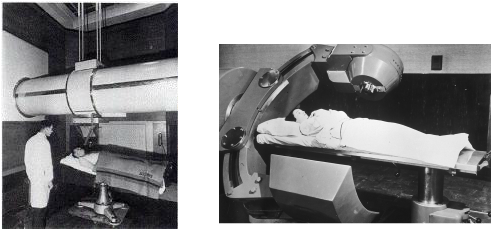
History Of Radiation Therapy:
|
[1] Radiation therapy (also known as radiotherapy) is the use of radiation to treat cancerous or benign tumors and other medical conditions. Often used with radiology, another medical specialty that uses low-energy X-rays to create images, radiation therapy uses high-energy X-rays to treat patients. The field of radiation oncology is one of the three pillars of cancer therapy, along with surgery and chemotherapy. Nearly two-thirds of cancer patients in the United States receive radiotherapy. It is also the most effective way to treat pain in cancer patients when a cure is no longer possible. The field of radiation therapy was born not long after the discovery of X-rays in 1895 by German Physicist Wilhem Roentgen. Radiation was influenced by electrotherapy and escharotics, doctors began using raditation to help treat growths produced by diseases such as epithelioma.
|
[1] In 1901, radiation therapy began with radium and with relatively low-voltage diagnostic machines. It was discovered that daily doses of radiation over several weeks greatly improved the patient's chance for a cure. Since then, the methods and the machines that deliver radiation therapy have improved.
At the beginning of the 20th century, shortly after radiation began to be used for diagnosis and therapy, it was discovered that radiation could cause cancer as well as cure it. Many early radiologists used the skin of their arms to test the strength of radiation from their radiotherapy machines. A related technique called conformal proton beam radiation therapy, uses a similar approach to focusing radiation on the cancer, but this time it's proton beams. Protons cause very little damage to the nearby tissues but are very effective in killing cancer cells when passing through. This means that proton beam radiation therapy can deliver more radiation to the cancer while not harming the tissues. |
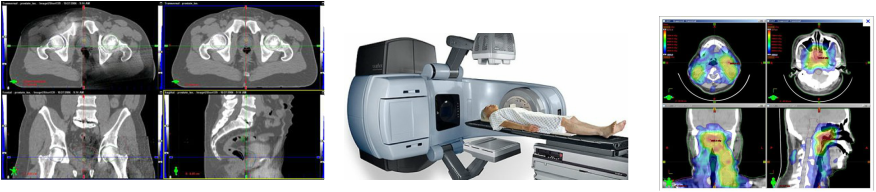
Development of Radiation Therapy:
[2] Over the past 100 years, radiation therapy has been improving with more treatments. Intensity-modulated radiation therapy (IMRT) is an advanced type of radiation therapy used to treat cancer and noncancerous tumors. IMRT uses advanced technology to manipulate photon and proton beams of radiation to conform to the shape of a tumor. This type of treatment is totally painless and won't attack the patient's tissues. Image-guided radiation therapy (IGRT) is the process of frequent two and three-dimensional imaging, during a course of radiation treatment, used to direct radiation therapy utilizing the imaging coordinates of the actual radiation treatment plan. IGRT is used to treat tumors in areas of the body that are prone to movement, such as the lungs (affected by breathing), liver, as well as tumors located close to critical organs and tissues. IGRT is similar to IMRT, they are both painless and won't attack the patient's tissues.
[3]Linac-based radiation therapy for cancer therapy began with treatment of the first patient in 1953 in London at Hammersmith Hospital, with an 8 MV machine built by Metropolitan-Vickers, as the first dedicated medical linac. A short while later in 1955, 6 MV linac therapy from a different machine was being used in the United States.
[3]Medical grade linacs accelerate electrons using a tuned-cavity waveguide, in which the RF power creates a standing wave. Some linacs have short, vertically mounted waveguides, while higher energy machines tend to have a horizontal, longer waveguide and a bending magnet to turn the beam vertically towards the patient. Medical linacs use monoenergetic electron beams between 4 and 25 MeV, giving an X-ray output with a spectrum of energies up to and including the electron energy when the electrons are directed at a high-density (such as tungsten) target. The electrons or X-rays can be used to treat both benign and malignant disease. The LINAC produces a reliable, flexible and accurate radiation beam. The versatility of LINAC is a potential advantage over cobalt therapy as a treatment tool. In addition, the device can simply be powered off when not in use; there is no source requiring heavy shielding – although the treatment room itself requires considerable shielding of the walls, doors, ceiling etc. to prevent escape of scattered radiation. Prolonged use of high powered (>18 MeV) machines can induce a significant amount of radiation within the metal parts of the head of the machine after power to the machine has been removed (i.e. they become an active source and the necessary precautions must be observed).
[3]Medical grade linacs accelerate electrons using a tuned-cavity waveguide, in which the RF power creates a standing wave. Some linacs have short, vertically mounted waveguides, while higher energy machines tend to have a horizontal, longer waveguide and a bending magnet to turn the beam vertically towards the patient. Medical linacs use monoenergetic electron beams between 4 and 25 MeV, giving an X-ray output with a spectrum of energies up to and including the electron energy when the electrons are directed at a high-density (such as tungsten) target. The electrons or X-rays can be used to treat both benign and malignant disease. The LINAC produces a reliable, flexible and accurate radiation beam. The versatility of LINAC is a potential advantage over cobalt therapy as a treatment tool. In addition, the device can simply be powered off when not in use; there is no source requiring heavy shielding – although the treatment room itself requires considerable shielding of the walls, doors, ceiling etc. to prevent escape of scattered radiation. Prolonged use of high powered (>18 MeV) machines can induce a significant amount of radiation within the metal parts of the head of the machine after power to the machine has been removed (i.e. they become an active source and the necessary precautions must be observed).
[1] "History of Radiation Therapy." UC San Diego Health Sciences. Web. 5 Jan. 2016.
[2] "Evolution of Cancer Treatments: Radiation." Evolution of Cancer Treatments: Radiation. Web. 5 Jan. 2016.
[3] "Linear Particle Accelerators". (n.d.). Retrieved January 6, 2016, from https://en.wikipedia.org/wiki/Linear_particle_accelerator#Medical_linacs
[2] "Evolution of Cancer Treatments: Radiation." Evolution of Cancer Treatments: Radiation. Web. 5 Jan. 2016.
[3] "Linear Particle Accelerators". (n.d.). Retrieved January 6, 2016, from https://en.wikipedia.org/wiki/Linear_particle_accelerator#Medical_linacs